Joint preservation refers to a set of operations that aims to preserve the articular cartilage (cartilage that lines the bone) or fill in an articular cartilage defect. What operation a patient gets depends on the location of the articular cartilage defect, and the size of the articular cartilage defect. Nigel will explain your MRI findings to you and what operation is best suited for your articular cartilage defect.
Types of Treatments
Stabilisation
Sometimes an articular cartilage flap can be stabilised using an absorbable pin.
For an operation like this to be performed there needs to be a piece of bone attached to the flap as this will provide a stable base for fixation. Stabilisation is most commonly performed in acute injuries to articular cartilage or for articular cartilage lesions in children.
Debridement
Debridement is where the articular cartilage is smoothed over either with a mechanical shaver or with a thermal cautery type device. The arthroscopy photo shows cracking or fissuring of the articular cartilage. This fissuring would be debrided with amechanical shaver. The arthroscopy photo on the right shows fibrillation and again this articular cartilage would be debrided using a mechanical shaver.

Micro-Fracture
Involves using a sharp instrument to make little holes in the bone that is exposed (the articular cartilage that was there has been removed). This stimulates your body to release substances into the knee, that fills the defect (hole) with a kind of cartilage that is not normal like the cartilage you had there before but will hopefully settle your symptoms. It is used for larger size defects of the articular cartilage.
ACI / MACI® and AMIC®
ACI (Autologus Chondrocyte Implantation) / MACI® (Matrix-induced Autologus Chondrocyte Implantation)
These techniques can be used for a medium sized defect of the articular cartilage (cartilage that lines the bones of the knee joint) on one side of the joint. It involves taking normal cartilage from somewhere in your knee (that does not form part of a moveable part of the joint) during an arthroscopy of your knee. It is then grown in a laboratory and at your second knee operation is implanted or put back into the knee where the defect (hole exists) in your knee.
Unfortunately ACI and MACI® are not rebatable, which means in the private health system the patient has to pay for the procedure. These costs are significant.
AMIC® (Autologus Matrix Induced Chondrogenesis)
Is a similar technique that is done with one operation only, is done arthroscopically. AMIC® is not rebatable. The short-term results of this procedure are encouraging but further follow-up needs to be performed to show that in the medium to long term AMIC® is an acceptable option for articular cartilage defects.
If Nigel feels you may benefit from one of these procedures he will discuss these options with you.
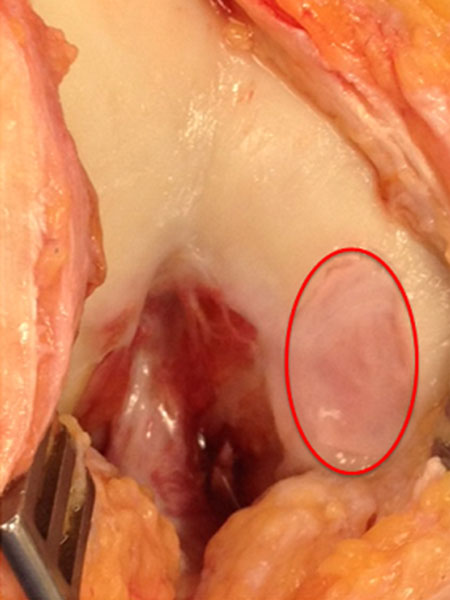
This photograph (below) is the second operation to implant the ACI or MACI graft into the defect. The graft tissue has been grown in a laboratory for 6 weeks and is marked with the red circle.
Articular Cartilage Transfer
Osteo-Articular Transfer System (OATS)
These are used for smaller size articular cartilage defects.
Mosaicplasty
As the name suggests multiple small articular cartilage plugs are placed into the defect and the appearance is of a mosaic.
These procedures take normal articular cartilage from areas of your knee that are not involved with weight bearing or with one bone moving over another and are placed into the area of the articular cartilage defect.
Mega-OATS and Osteochondral Allograft Transplantation (OCA)
Used for large defects in the articular cartilage and uses donor (cadaver) articular cartilage. These procedures are done rarely and you have to fulfill a strict set of criteria. If Nigel feels you are a candidate for this procedure he will discuss these options with you.
What to Expect – Pre & Post Surgery Joint Preservation
Arthroscopy
Arthroscopy of the knee is performed through two small incisions (cuts) made on the front of the knee. This allows the fibre-optic camera to be passed into one of the incisions and instruments to do the operation going in the other incision.
It is generally day-case surgery. Arthroscopy is the main stay of addressing articular cartilage defects
Prior to Surgery
You will be given an information pack on joint information and arthroscopy on the day you are booked for surgery. Most joint preservation procedures are carried out as a day case however rarely, you may require an overnight stay.
It is unusual that extra tests will be required however Nigel will ask if you:
- have any medical conditions
- are on any medications
- have any allergies which may mean you may need to have further tests or be referred to a physician for further assessment
On the day of surgery
- You will not meet the Anaesthetist generally until just prior to surgery.
- If you take any blood thinning medication, please tell Nigel as in certain cases you may need to stop this medication for a period of time prior to surgery.
- You must have nothing to eat or drink for at least 6 hours prior to surgery.
- Your leg will be washed with an antiseptic solution.
- Nigel will come and have a talk with you and place a mark on the correct limb that is going to be operated on.
- Nigel’s assistant surgeon will introduce themselves to you.
- A physiotherapist will meet with you to give you crutches, simple exercises to do following surgery, and answer any other questions you may have.
- In most cases surgery is carried out under a general anaesthetic.
In surgery
- You will have an intra-venous (IV) line placed into a vein in your hand or forearm.
- You will be given oxygen to breathe and the Anaesthetist will then drift you off to sleep.
- A final check will be done to confirm all your details are correct, that the correct limb is marked, and the correct operation is being performed.
- A tourniquet will be placed around your thigh to restrict blood flow to the knee, to enable the operation to be performed.
- No antibiotics will be given unless deemed necessary.
- Your leg will be washed again with an antiseptic solution and then surgical drapes will be placed around your limb and body.
- Two small cuts will be made at the front of your knee so that the arthroscope is introduced into the knee.
- If you are having a transfer procedure a larger cut will be made on the inside of your patella (knee cap).
- The operation will then be performed.
- Initially a thorough examination is made of the entire knee and then particular reference is made to the problem as discussed with Nigel.
- At the end of the operation local anaesthetic will be placed into the knee joint and also into the incisions (cuts) at the front of your knee.
- The incisions (cuts) around the front of your knee will be steri-stripped together and a tubigrip stocking placed over your knee.
- You will then be taken to the recovery room and eventually back to the day surgery unit.
Immediately after surgery
- You will wake up in recovery.
- You will feel some discomfort in your knee, which should be easily managed with painkillers or an anti-inflammatory medication.
- You will be encouraged to get up and about, and walk.
- You may need to use crutches for up to a week in some cases or longer depending on what operation was done and Nigel will tell you what your weight-bearing status is post-surgery.
- Photographs and video are taken of your knee during the operation which will be given to you as a DVD.
You will find 2 small puncture wounds under the dressing covering your knee, which are closed bysteri-strips (or occasionally sutures). These wounds are small, but the surgery inside your joint is significant and your knee will take time to recover. It is important that you follow the instructions on this sheet to help healing, to maintain muscle strength and movement of your knee.
Nigel will have a chat with you after your operation to discuss the findings of your joint preservation procedure.
An appointment card will be given to you to see Nigel 2-3 weeks following your operation.
Post-Surgery
For the first 3-4 days you need to elevate your knee (sitting in bed/couch). Ice your knee regularly and do light exercise. By day 3 you may start to walk around more.
Progress
It is important not to push your knee too hard, as this will slow healing. Signs that you are doing too much include: increased swelling / pain / stiffness temperature in the joint.
Puncture Wounds
This area should remain dry until the steri-strips are removed 10-14 days post- operation. These areas may be slightly tender and puffy for 1-2 months post- operation and will benefit from gentle massage once healed. The area should remain dry until the steri-strips are removed 10-14 days post- operatively. Wrap a plastic bag / glad-wrap / cling-film around your knee when showering.There may be some bleeding from the puncture sites. This is nothing to worry about in general. Excessive bleeding may require re-dressing. Please call the hospital where the surgery was performed or Nigel’s rooms if this occurs.
Swelling
The amount of swelling following joint preservation varies and tends to be dependent on the pre-operative state of your knee, and how much is done to your knee during surgery. An increase in the amount of swelling in the early post-operative days indicates that you are doing too much. It is important to decrease the amount of swelling as quickly as possible.
This can achieved by:
- Not overdoing things
- Using crutches to reduce the weight
- Keep the leg elevated as much as possible
- Using a compression bandage
- Using ice at regular intervals
- You should check your leg frequently to ensure that it is pink in colour and NOT white or blue, as this may indicate ice burn. You may apply ice (wrapped in a wet towel) 3-4 hourly, for 30-minutes duration. (Frozen vegetables can be used). Please use a barrier between the skin and the ice.
Pain
- The most important part after your surgery is to keep your pain under control. This is done with medications.
- The anaesthetist will give you a script for pain- killers and an anti-inflammatory if you do not already have them.
- The medication needs to be taken regularly especially for the first 4 days.
- If your pain is not controlled by the medication, please call Nigel’s rooms.
Crutches
Crutches are to be used to control weight bearing transmitted through your knee.
Stairs
Walking and movement are encouraged to help get the knee moving. It is extremely important to use crutches when you negotiate stairs.
Remember this sequence
- WHEN GOING UPSTAIRS: Good leg, operated leg, then crutches.
- WHEN GOING DOWNSTAIRS:Crutches, operated leg, then good leg
Driving
Nigel will discuss with you when you can return to driving.
Work
Work activities depend on the job that you do and Nigel will advise you of an appropriate time to return to your work. If you work in an office you may then return to work when you are able. Active jobs will need longer periods off work up to 8 weeks for manual labourers.
Sports
Sports activities should not be attempted before 6 months at the earliest but again Nigel will advise of when you can return to these.
Complications
Bruising
Bruising is common following arthroscopy and may occur around the top part of your thigh (where the tourniquet was), in your calf, or around your knee. It may take 2 weeks for this to settle down.
Swelling
Your knee can be swollen for up to 12 weeks, and does depend on how much work was done in your knee joint. Swelling reduction with ICE is important and should be done regularly for the first 10-14 days.
Infection
Is less than 0.5% (1/200).
It is important to seek medical advice if you have any of the following:
- Feel unwell
- Increased pain in your knee or with movement
- Increased heat or redness around your knee
- Increased swelling of your knee
- If there is a creamy discharge from the wounds
- If you experience discomfort or feel lumps in your groin
Any of these symptoms may indicate that you have an infection and it is important to seek medical advice as soon as possible
Blood clots (DVT)
Occur in 10-15% of patients having an arthroscopy of the knee.
Most cases are not picked up and do not cause problems.
But if you have:
- Increased pain or discomfort in your calf
- Increased swelling of your calf
- Increased pain with movement of your calf
- Your breathing pattern changes or you feel short of breath
Any of these may suggest you have a blood clot and you should seek medical advice as soon as possible.
Ongoing pain
Some patients may still have pain following surgery. This is not uncommon particularly in those who have arthritis (wear and tear) in their knee or those who have inflammation of their knee.
The locking or catching sensation will go but the pain may remain.
Recurrence of symptoms
In some cases symptoms will recur and the articular cartilage may degenerate.
Important Note:
You may have discomfort, swelling, bruising and/or clicking in your knee for up to 8 weeks after your operation. These are normal occurrences post operation. However, after 8 weeks if you continue to have any of those symptoms please contact Nigel’s rooms. It is important not to overdo things after your operation as you may cause damage to your knee.



